A single reading can be misleading. Learn what blood pressure is considered high, how to re-check correctly, and what patterns are worth following up on.
Most people don’t search “when is blood pressure high” after a great reading. They search for it after a number that surprises them.
Here’s the calming truth: one blood pressure reading is a snapshot. It tells you what was happening in one moment, under one set of conditions. Blood pressure naturally moves throughout the day, and small factors like stress, sleep, caffeine, timing, and even how you’re sitting can shift the number.

Medical Grade, Accurate, FDA-Cleared Heart Insights.
Save 20% on checkout with code VITALITY
That’s why clinicians don’t label blood pressure “high” based on a single reading alone. They look for repeatability under consistent conditions, and for patterns that hold over time. That’s also why guidelines recommend confirming high office readings with measurements outside the clinic before starting treatment.
So the goal isn’t to obsess over every spike. It’s to figure out whether your blood pressure is showing a true trend in the wrong direction, or just a normal fluctuation.
If you want a quick refresher on what 120/80 represents, here’s a simple explainer: What does 120/80 mean?
Reference ranges, at a glance
In the U.S., blood pressure is often discussed using American Heart Association (AHA)/American College of Cardiology (ACC) guideline categories. The chart below is an AHA visual summary of those categories that can help place a reading quickly. These categories are best used as reference points, not a diagnosis from one measurement.
Use the chart for quick context. Then we’ll show how to re-check a surprising reading so you can tell whether it’s a one-off or a real pattern.
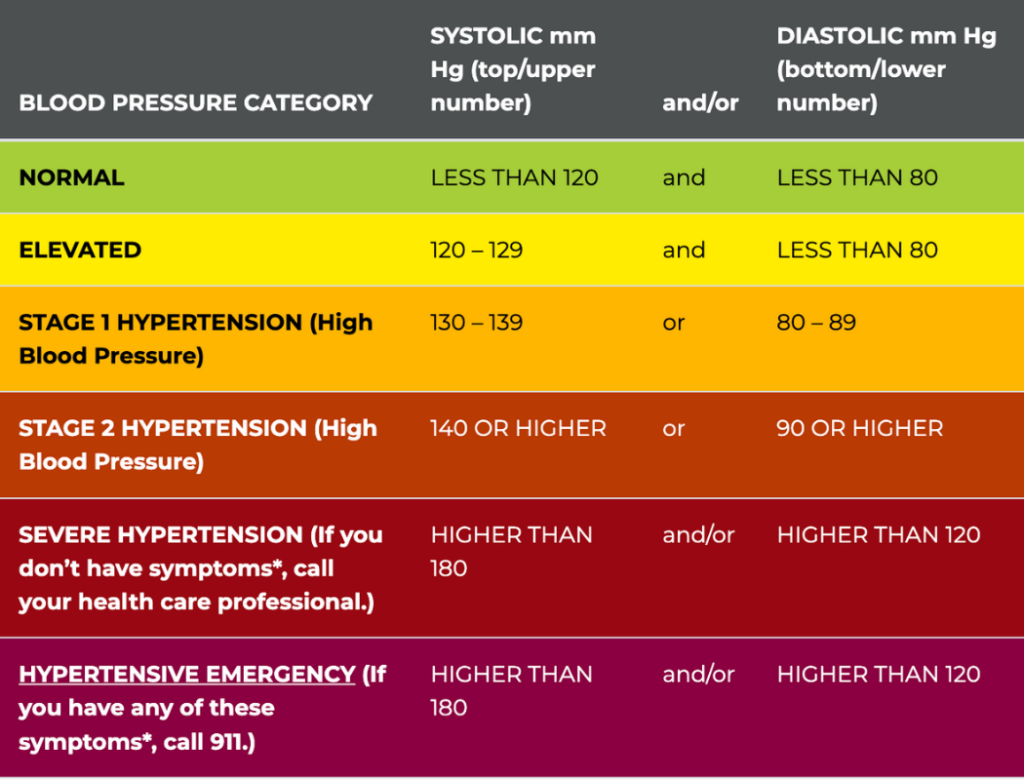
Here’s the key takeaway: a single reading can land in a higher category and still not represent your typical blood pressure. What matters is what your numbers do when you measure correctly and consistently across multiple checks.
Why you may see different cutoffs
In the U.S., many references use 130/80 as the starting point for “high” categories. In parts of Europe, you’ll often see 140/90 used as the hypertension cutoff.
Different frameworks, same takeaway: measure correctly and look for patterns over time.
How to re-check correctly, so you don’t chase noise
Once you’ve placed a reading in context, the next step is simple: re-check it in a way you can actually trust.
Blood pressure can shift based on small, everyday factors. If you take a reading right after rushing around, while you’re talking, or before you’ve fully settled, you may capture a number that reflects the moment more than your true baseline.
A good re-check doesn’t need to be complicated. It just needs to be consistent.
A simple re-check routine
Set up consistently. Sit quietly for a few minutes. Keep your feet flat on the floor, your back supported, and your arm resting comfortably at about heart level. Avoid talking during the reading.
Take two readings. Check your blood pressure, wait about a minute, then take a second reading. If the first number was unusually high, the second often gives you a clearer picture.
Record what you see. Note the numbers and any obvious context that could matter, such as poor sleep, stress, caffeine, alcohol, exercise, or travel. You don’t need to track everything. Just enough to recognize patterns later.
Repeat under the same conditions. If you’re trying to understand whether your blood pressure is truly running high, the most useful comparisons come from readings taken at roughly the same time of day, in a similar setting, using the same method.
For a broader look at good home measurement habits, the checklist in our 120/80 article is a useful reference.
The goal here is not to “prove” you have a problem or convince yourself you don’t. It’s to reduce noise so you can see whether a higher reading was a one-off spike or part of a real trend worth following up on.
Home vs. the doctor’s office: why your numbers can differ
Even when you measure correctly, it’s common to see different numbers at home than you see in a clinic.
For some people, blood pressure runs higher at the doctor’s office because of stress, rushing, or the simple pressure of being in a medical setting. That is often called the “white coat” effect. In that case, home readings may give a more realistic picture of what your blood pressure looks like day to day.
For others, the opposite happens. A reading at the doctor can look normal, while blood pressure runs higher in everyday life. This pattern is sometimes called “masked” hypertension. It can happen when day-to-day conditions outside the clinic differ from the calmer environment of an appointment.
The important point isn’t to decide which environment is “right.” It’s to recognize that a single clinic reading may not reflect your typical pattern, which is why repeat measurement over time can be so valuable.
If you’re seeing big differences between home and clinic readings, focus on consistency at home and bring your log to your next appointment. It helps your clinician see what’s typical for you, not just what happened in one moment.
What patterns matter most
Once you’re measuring consistently, the question shifts from “what did I get today?” to “what is my blood pressure doing over time?”
Start with your average trend. One high reading can happen. What changes the conversation is when your usual range is consistently elevated across multiple checks. If your baseline is drifting upward week over week, that matters more than any single spike.
Next, pay attention to how often higher readings repeat under similar conditions. If you’re seeing elevated numbers only after poor sleep or a stressful day, that’s useful context. If the same pattern shows up even when you’re well rested and calm, that’s a stronger signal it may be worth following up.
Finally, watch for consistency in your measurement routine. The more consistent the conditions, the easier it is to tell whether a pattern is real or whether you’re just seeing noise. Timing, posture, talking, recent caffeine or exercise, and even cuff fit can all affect the result.
Consistent measurement is easier when you have a tool built for it. CONNEQT Pulse captures readings and tracks trends over time, so the pattern becomes visible without having to piece it together manually. That’s the practical difference between knowing what your blood pressure did today and understanding what it’s been doing over weeks and months.
The goal isn’t to make every reading perfect. It’s to understand what’s typical for you, spot meaningful changes early, and respond based on a pattern instead of a moment.
When it’s worth following up
If your readings are occasionally higher but return to your usual range when you re-check calmly and consistently, that may be normal variation.
What’s more important is when a higher pattern holds. If your blood pressure stays elevated across multiple days, despite using a consistent method and similar conditions, it’s worth discussing with a clinician. Bringing a simple log of your readings and the circumstances around them can make that conversation much more productive.
It’s also worth following up sooner if your numbers are repeatedly very high, or if you have symptoms that concern you. In those cases, the safest move is to seek urgent care when appropriate and follow up with a healthcare provider. If you don’t have one, finding a primary care physician is a worthwhile first step.
The goal here isn’t to diagnose yourself. It’s to recognize when a pattern deserves attention, so you can address it early rather than ignoring it for months or years.
Put it together: a calm, repeatable framework
If you take away one thing from this article, let it be this: a single blood pressure reading is rarely the full story. What matters is what your numbers do when you measure consistently over time.
Here’s a simple way to approach it:
1) Measure the right way, every time.
Sit, rest, and follow the re-check routine above. Consistency is what makes the data useful.
2) Look for a pattern.
Pay attention to your typical range, not your best or worst moment.
3) Follow up when a pattern persists.
If a higher baseline holds, bring your log to your clinician and discuss next steps.
This approach keeps you out of the extremes. It helps you avoid overreacting to one number, while also making sure you don’t ignore a trend that deserves attention.
What to read next
If you want to go deeper, these articles can help you interpret your blood pressure readings with clearer context and understand what influences them over time: