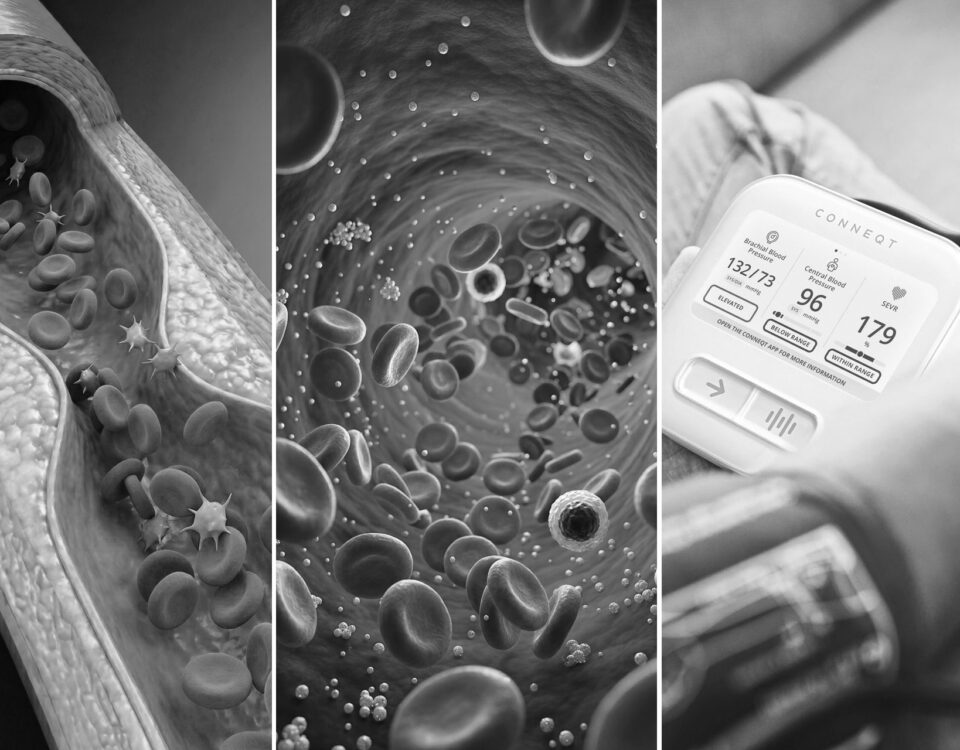
Cardiovascular disease doesn’t begin with a diagnosis. It begins in the arterial wall, through changes that are often detectable before standard tests raise a flag. Here’s what those changes are, why they matter, and what earlier visibility can do for you.
Most people think about cardiovascular health in terms of events. A high blood pressure reading. An abnormal test result. A symptom that finally prompts a doctor visit.
But the biological process that leads to those moments begins much earlier, in the arterial wall itself.

Medical Grade, Accurate, FDA-Cleared Heart Insights.
Save 20% on checkout with code VITALITY
These changes develop gradually, over years, through a process that is often detectable before standard tests flag anything unusual. In people who feel completely well.
That’s not meant to be alarming. It’s meant to be useful. If change builds gradually, that same timeline creates a window for awareness, for measurement, and for the kind of informed conversations with your clinician that are most valuable before a problem becomes harder to address.
This guide explains what those early changes are, what the research shows about when they begin, and what consistent measurement can reveal that a single office visit often can’t.
In this article
- The earliest changes: endothelial function
- Early signs of arterial stiffness: what to know
- What the research shows about timing
- Why standard measurements miss this
- What you can do with this information
- Quick recap
- What to read next
What healthy arteries actually do
Your arteries do more than carry blood from one place to another. They are active, responsive structures that expand and contract with every heartbeat, absorbing pressure and regulating flow.
That flexibility matters. When the heart pumps, it generates a pressure wave that travels through the arterial wall. Healthy, elastic arteries absorb and buffer that wave. That reduces the load on the heart and protects the smaller vessels and organs downstream. The brain, kidneys, and heart itself are all sensitive to that force over time.
At the center of that function is the endothelium, a thin layer of cells lining the inside of every artery. It does much more than act as a barrier. The endothelium actively regulates how arteries respond to changes in blood flow, helps control inflammation, and plays a direct role in how well arteries dilate when demand increases.
When this system is working well, the heart doesn’t have to work as hard. Pressure is buffered before it reaches sensitive organs. The body handles stress efficiently.
Understanding this baseline is what makes the early changes worth paying attention to.
The earliest changes: endothelial function
Before arteries show measurable structural change, something more subtle shifts first.
The endothelium, the inner lining of the arterial wall, begins to respond differently. In a healthy artery, increased blood flow triggers a signal that causes the artery to dilate. That dilation is a sign of a well-functioning vascular system.
When endothelial function declines, the artery becomes less responsive. It doesn’t dilate as readily. The system starts to lose some of its adaptability.
This can happen in people who feel completely well, with blood pressure and cholesterol levels that haven’t yet raised any flags. It’s one of the earliest detectable signs that the arterial wall is under stress, often appearing before structural changes like arterial stiffness become measurable.
How researchers measure it
Researchers measure endothelial function using a test called flow-mediated dilation, or FMD. It works by briefly restricting blood flow to the forearm and then measuring how much the artery dilates when flow is restored. A healthy artery dilates readily. A less responsive artery dilates less.
FMD isn’t part of standard preventive care in the US. But the research behind it is meaningful. Studies in people free of cardiovascular disease at baseline found that FMD was associated with future cardiovascular events in people who had no established disease at the time of measurement.
It helps to understand the sequence. Endothelial dysfunction tends to develop first. Over time, if the underlying drivers persist, the arterial wall itself begins to change structurally, becoming stiffer and less elastic. That structural change is what the next section covers. And it’s that stiffening, over years, that can eventually contribute to rising blood pressure and, later still, to clinical events.
The process is gradual. And because it’s gradual, it creates a window.
A conversation worth having with your clinician
FMD testing, the endothelial function measure described above, isn’t something most people will encounter at a standard checkup.
But if you have a family history of early cardiovascular disease or risk factors that don’t fully explain your cardiovascular history, endothelial function testing may be worth raising with your clinician. The same is true if you simply want a more complete view of your vascular health.
It reflects vascular biology rather than a specific diagnosis, but for some people, it can be an informative conversation starter.
Early signs of arterial stiffness: what to know
As endothelial function declines over time, the arterial wall itself begins to change. It becomes less elastic, less able to absorb the pressure wave generated by each heartbeat.
That structural change is what we call arterial stiffness, and its early signs can appear long before blood pressure rises or standard tests flag a concern. It’s also one of the most studied early signals in cardiovascular research.
Stiff arteries transmit pressure rather than absorbing it. More force reaches the heart, the brain, and the kidneys with every beat. Over time, that added strain matters.
How arterial stiffness is measured and what it predicts
Researchers measure arterial stiffness using a metric called pulse wave velocity, or PWV. The concept is straightforward: the stiffer an artery, the faster a pressure wave travels through it.
PWV has been studied in large, long-term community populations. In people free of cardiovascular disease at the start, elevated arterial stiffness independently predicted the development of hypertension, cardiovascular events, kidney disease, and other conditions over follow-up periods of up to 20 years. That association held even after accounting for standard risk factors like blood pressure and cholesterol.
One finding is particularly relevant here. Research shows that arterial stiffness can precede and contribute to the development of hypertension, not merely accompany it. The arterial wall can stiffen before blood pressure rises to concerning levels. The structural change comes first.
Population research gives us a sense of what these numbers look like across healthy adults. PWV typically averages around 7 to 8 meters per second in midlife and rises with age. International cardiovascular guidelines recognize values above 10 meters per second as associated with elevated risk. These are reference points drawn from large population studies, not thresholds for individual diagnosis. They help put the signal in context.
What the research shows about timing
The changes described in the previous two sections don’t happen overnight. They develop over years, sometimes decades, before they show up in standard clinical measurements.
Long-term research gives us the clearest picture. The Framingham Heart Study followed thousands of community participants, free of cardiovascular disease at the start, for up to 20 years.
People who had elevated arterial stiffness at midlife were more likely to develop hypertension, cardiovascular events, and kidney disease over the decades that followed. That association held even after accounting for standard risk factors.
That’s a long runway. It’s also a meaningful one.
Other research has looked at the sequence more closely. Arterial stiffness doesn’t just accompany hypertension. It can precede and contribute to it. The arterial wall stiffens first. Blood pressure rises later.
That matters. It means the earliest measurable changes may occur before the most commonly tracked clinical marker moves at all.
The honest framing is a trajectory, not a countdown. No single study cleanly quantifies how many years before symptoms arterial changes begin in any given person. What the research does show is that the gap between early change and clinical event is measured in years to decades.
That timeline cuts both ways. The same gradual process that creates risk also creates opportunity. Earlier awareness and earlier measurement are most valuable precisely because of that window.
Why standard measurements miss this
A standard blood pressure reading is valuable. It captures an important signal and it’s the foundation of cardiovascular risk assessment for good reason.
But it measures pressure at the arm. And what happens at the arm isn’t always the same as what happens closer to the heart.
That gap matters more than most people realize.
The pressure wave generated by the heart changes as it travels outward through the arterial system. In young, elastic arteries, that wave is amplified as it moves away from the heart. In stiffer arteries, that amplification is reduced. The result is that two people can have similar readings at the arm while experiencing very different pressure loads closer to the heart.
Central blood pressure, the pressure closer to the aorta, reflects what the heart and organs are actually experiencing. It can differ meaningfully from the brachial reading taken at the arm.
When normal readings can mask elevated pressure
This is where the gap between standard and central measurement becomes most concrete.
Research has identified a group of people with a condition sometimes called isolated central hypertension. These are people whose brachial blood pressure looks normal but whose central blood pressure is elevated.
It’s a relatively small group, estimated at around 4% of the population. But that group carried more than twice the cardiovascular event risk of people whose readings were normal on both measures.
They would have been missed by a brachial reading alone.
This isn’t a reason to distrust standard blood pressure measurement. It’s a reason to understand what it captures and what it doesn’t.
A single office reading is a snapshot. Central blood pressure and arterial stiffness add depth to that picture. They reflect what’s happening in the arterial wall, not just at the surface.
What you can do with this information
Understanding that arterial changes can precede symptoms by years is useful. But only if it translates into something practical.
The good news is that it does.
Awareness changes how you think about cardiovascular health
Most people approach heart health reactively. A concerning reading prompts a conversation. A symptom prompts a visit.
Earlier awareness shifts that framing. It doesn’t mean obsessing over every number. It means understanding that the cardiovascular system sends signals before it sends symptoms. And that those signals are worth paying attention to.
Consistent measurement creates visibility
A single reading is a snapshot. A pattern is information.
Blood pressure tracked consistently over time reveals things a single office visit can’t. Whether your baseline is stable. Whether it’s drifting. Whether lifestyle changes are moving it in the right direction.
Central blood pressure and arterial stiffness go deeper. They reflect what’s happening closer to the heart, not just at the surface. And they can be tracked at home, consistently, over time.
Home measurement over time can help close the gap between annual checkups and daily cardiovascular reality.
Standard home monitors measure pressure at the arm, known as brachial blood pressure. The CONNEQT Pulse goes further. Using pulse wave analysis, it tracks central blood pressure and arterial stiffness: two of the signals this article has been building toward. Not as a diagnostic tool. As a way to build visibility into how your cardiovascular system is changing over time.
The conversation with your clinician gets better
Arriving at an appointment with a pattern rather than a single number changes the conversation.
It gives your clinician more to work with. It makes the discussion more specific. And it puts you in a better position to ask the right questions and understand the answers.
Questions worth bringing to your next appointment
Starting a conversation about arterial health doesn’t require knowing all the answers. There are a few questions worth considering:
- Has my arterial stiffness ever been measured?
- Would central blood pressure monitoring make sense given my history?
- Are there risk factors in my picture that standard measurements might not be capturing fully?
These aren’t demands for specific tests. They’re starting points for a more complete conversation about your cardiovascular health.
Quick recap
Cardiovascular disease doesn’t begin with a diagnosis. It begins in the arterial wall, through changes that are often detectable before standard tests flag anything unusual.
Here is what this guide covered:
- Healthy arteries are active and flexible. They absorb pressure, regulate blood flow, and protect the heart and organs downstream. That function matters.
- Endothelial function shifts first. Before arteries stiffen structurally, their inner lining becomes less responsive. This is one of the earliest detectable signs of arterial stress, often appearing before standard markers change.
- Arterial stiffness is the next measurable shift. Measured by pulse wave velocity, it can precede and contribute to hypertension, not merely accompany it. The structural change comes first.
- The timeline is years to decades. Long-term research shows that elevated arterial stiffness at midlife consistently pointed toward worse outcomes later. That same gradual timeline also creates a window for earlier awareness.
- Standard measurements capture part of the picture. Central blood pressure and arterial stiffness add depth that a brachial reading alone can’t provide.
- Earlier visibility changes what’s possible. Consistent measurement, informed conversations with your clinician, and tracking the right signals over time are most valuable precisely because of that window.
What to read next
If you want to go deeper, these articles can help you understand the signals this guide introduced and what to do with them over time.
- Why Your Blood Pressure Readings Fluctuate, and What to Do About It – How to measure consistently and make sense of patterns over time.
- When Is Blood Pressure Actually High? – A practical way to think about “high,” how to re-check, and what patterns are worth following up on.
- Why 120/80 Is a Clinical Reference, Not Just a Number – What 120/80 actually represents and why it’s a reference point, not a personal scorecard.
- Fit, Healthy, and Still at Risk? What ApoB Reveals That LDL Misses – Another signal worth understanding — and why standard labs don’t always tell the full story.
Want to explore more heart health articles? Browse the full library.