My Cleerly scan came back clean. Zero plaque. My calcium score is zero. My arterial function is strong. And none of that tells the full story.
Six years ago, my PCP looked at my calcium score and told me I was fine.
Zero calcified plaque. Clean bill of health. No follow-up needed.

Medical Grade, Accurate, FDA-Cleared Heart Insights.
Save 20% on checkout with code VITALITY
By every conventional measure, my cardiovascular system looked like it was doing exactly what decades of consistent training are supposed to produce.
I accepted that. It made sense at the time.
What I have learned since then is that the cardiovascular risk profile of a fit, high-volume athlete is genuinely different from both a sedentary person and someone who exercises moderately.
Not worse, necessarily. But different in ways that standard screening was not designed to detect.
That difference has a name. It is called the athlete phenotype. And understanding it changed how I think about my own risk entirely.
In this article
- The calcium score pattern in athletes
- The mechanism question you are actually asking
- Why standard risk frameworks read the athlete profile incorrectly
- What I am actually monitoring and why
- What this means for fit athletes thinking about their own risk
- What to read next
What we mean by the athlete phenotype
The athlete phenotype is not a diagnosis. It is a description.
It refers to the cluster of adaptations that develop in people who train consistently at high volume or intensity over years and decades. Enlarged heart chambers. Lower resting heart rate. Greater stroke volume. Higher VO2 max. In many cases, more elastic arteries.
These are genuinely protective adaptations.
The evidence for consistent exercise as a cardiovascular protective factor is overwhelming, and I am not here to argue against it.
Training hard, done right, builds a more resilient cardiovascular system. That is not in question.
What is less well understood is that the athlete phenotype also produces some patterns that standard risk frameworks were not built to interpret.
The clearest example is the calcium score.
Fit male athletes, particularly those who have trained at high volume for decades, consistently show higher coronary artery calcium scores than matched sedentary controls. Not slightly higher. Significantly higher.
And this happens despite lower conventional risk factors, better fitness markers, and lower Framingham risk scores across the board.
That is the paradox at the center of this article.
If you train at this level, it is worth understanding too.
The calcium score pattern in athletes
The research on this is consistent enough that it has its own name: the athlete paradox.
Multiple studies have established that male masters endurance athletes show significantly higher coronary artery calcium scores than matched sedentary controls, despite lower Framingham risk scores, better metabolic markers, and the kind of cardiovascular fitness profile that standard risk models treat as protective.
The calcium score was supposed to be the reassuring number.
For a lot of high-volume male athletes, it is not.
My own score is zero. It was zero six years ago when my PCP cleared me. My recent Cleerly scan reaffirmed it. Cleerly is a coronary CT angiography scan that uses AI analysis to image both calcified and non-calcified plaque, going further than a standard CAC scan. Zero across the board.
That should settle it.
It doesn’t.
Because my zero score raises the same mechanistic question the paradox raises for athletes who do have elevated CAC: what is actually driving the pattern, and does my profile put me on a trajectory toward it?
It is the right question to be asking.
One note on female athletes. The athlete paradox appears to be predominantly a male finding. A 2024 study in Circulation found no elevated CAC in female masters endurance athletes compared to sedentary controls.
That distinction matters for how you read everything that follows.
The mechanism question you are actually asking
If fit athletes develop more calcified plaque, what is driving it?
That is the question I kept coming back to. Not whether the pattern exists. The research on that is clear. But why it exists, and what the mechanism actually tells you about risk.
The honest answer is that researchers have identified several candidate mechanisms. They are not mutually exclusive. They may all be operating simultaneously.
Here is what the evidence currently supports.
Mechanical stress on the arterial wall
High-volume exercise puts repeated hemodynamic stress on the coronary arteries.
During vigorous activity, blood flow through the coronary arteries becomes turbulent rather than laminar. Laminar flow is smooth and even. Turbulent flow creates uneven shear stress on the endothelium, the thin inner lining of the arterial wall. Over years and decades of high-volume training, that repeated mechanical stress may cause endothelial damage.
The body’s response to that damage is repair. And one form that repair takes is calcification.
This is the calcification-as-stabilization hypothesis. The body may be calcifying soft plaque more rapidly in athletes as a protective response, which would explain why athlete plaque tends to be more calcified and more stable than the mixed or non-calcified plaque seen in sedentary individuals with similar CAC scores.
It does not mean the plaque is not there. It means the body is handling it differently.
Inflammatory and oxidative stress
Acute strenuous exercise triggers a significant physiological response.
Inflammatory cytokines, reactive oxygen species, and oxidized LDL all enter the bloodstream during and after hard training sessions. In the short term this is part of the adaptive process. In the long term, at very high training volumes, the cumulative effect on the arterial wall is less well understood.
What the research suggests is that this repeated oxidative stress may contribute to atherosclerotic formation and progression over time, even in people whose resting inflammatory markers look clean.
My own resting inflammation markers are low. That matters. But resting markers capture one moment. They do not capture what happens during and after two hours at high intensity.
Parathyroid hormone and calcium metabolism
This one is less intuitive but worth understanding.
Vigorous exercise transiently elevates parathyroid hormone. PTH plays a central role in calcium metabolism, and post-exercise elevations in PTH have been shown to modify both the amount and the morphology, meaning the structure and composition, of calcific plaque in the coronary arteries.
This is an emerging area of research rather than a settled mechanism. But it adds another layer to why the calcium score in athletes may reflect something different from the calcium score in a sedentary person with conventional risk factors.
Three mechanisms. Potentially operating together. And none of them require elevated blood pressure, elevated blood sugar, or the conventional metabolic risk factors that standard screening is designed to detect.
That last point is the one I keep coming back to.
Those three mechanisms explain why athletes develop more calcified plaque. They do not fully explain my specific situation. Because alongside the athlete phenotype, there is a second framework that changed how I think about my ApoB and LDL-C numbers.
It is called the Lean Mass Hyper-Responder phenotype or LMHR.
What LMHR actually means
LMHR describes a specific metabolic pattern observed in lean, highly active, metabolically healthy individuals who show elevated LDL-C and ApoB despite excellent markers across the board.
Low triglycerides. High HDL. Low inflammation. Good insulin sensitivity.
My profile fits that pattern.
The proposed mechanism is called the lipid energy model. In lean, active individuals with low body fat and high energy demands, the liver upregulates production of LDL particles to transport triglycerides as fuel to peripheral tissues. Because there is little stored fat to draw on, the liver compensates by producing more cholesterol-carrying particles.
In plain terms, the liver is working efficiently to fuel a high-demand system. The byproduct is elevated particle traffic.
This means my elevated ApoB may not be the same signal as elevated ApoB in a metabolically unhealthy person. The origin is different. The mechanism is different. And the clinical implications may be different, though the research has not yet fully resolved what that means for long-term risk.
What the research shows about LMHR and plaque
This is where it gets genuinely interesting.
A 2024 cross-sectional study published in JACC: Advances examined 80 LMHR individuals with a mean LDL-C of 272 mg/dL for nearly five years. It compared their coronary plaque burden to matched controls with LDL-C of 123 mg/dL.
No significant difference in plaque burden between the two groups.
No correlation between LDL-C level and plaque burden in either cohort.
That is a striking finding. It does not mean elevated LDL-C in an LMHR context carries no long-term risk. Cross-sectional data has real limitations. But it does suggest that the standard assumption, that higher LDL-C equals more plaque, may not apply uniformly across metabolic phenotypes.
Here is where the uncertainty sits.
The LMHR research is promising but it is not settled science. The lipid energy model is a proposed mechanism with supporting evidence, not a proven causal chain. Cross-sectional data tells you where things stand at a point in time. It cannot tell you what happens over the decades ahead.
Two separate explanations for the same elevated number. Potentially interacting. The research does not yet tell us how.
What I can say is that the picture requires more tools and more nuance than a standard lipid panel can provide.
That is what I am working with. And it is why I track what I track.
Why standard risk frameworks read the athlete profile incorrectly
Standard cardiovascular risk calculators were built on general population data.
Not athletes. Not people who have trained at high volume for decades.
The Framingham risk score, the pooled cohort equations, the standard lipid thresholds. All of them were developed in populations that look nothing like a 62-year-old who trains seven days a week and has done so for most of his adult life.
That creates a specific problem.
These frameworks assign protective weight to exercise. And exercise is protective. But they were not designed to account for the specific cardiovascular pattern that develops at the upper end of the training volume distribution.
They treat high fitness as unambiguously favorable.
The athlete phenotype is more complicated than that.
The result is a risk picture that may be systematically misread in high-volume athletes.
The lipid framework has the same problem
For me, the misread runs deeper than that.
Because the standard lipid risk framework has a second problem when applied to someone with the LMHR metabolic pattern.
Elevated ApoB and LDL-C in a metabolically unhealthy person is a different signal from the same numbers in a lean, insulin-sensitive, highly active person whose liver is upregulating particle production as a fuel transport response.
The standard framework treats both numbers the same way.
A 2024 study published in JACC: Advances found no correlation between LDL-C levels and plaque burden in LMHR individuals, even at a mean LDL-C of 272 mg/dL over nearly 5 years.
That challenges the assumption that the standard LDL-C-to-atherosclerosis relationship applies uniformly across all metabolic phenotypes.
It does not settle the question. But it shifts it.
I sit at the intersection of two phenotypes that standard screening was not designed to read. The athlete phenotype on one side. The LMHR metabolic pattern on the other.
Each one individually creates readings that standard frameworks may misinterpret. Together, they create a risk picture that requires more nuanced tools and more specific markers than a standard lipid panel or calcium score can provide on their own.
This is not an argument against exercise. It is not an argument against taking lipid markers seriously.
It is an argument for monitoring that actually matches the profile.
What I am actually monitoring and why
Understanding the athlete phenotype and the LMHR pattern changed what I pay attention to.
Not because my numbers looked alarming. Because I started asking better questions about what my numbers actually meant.
The lipid markers that changed my thinking
My ApoB came back at 110 mg/dL.
By standard lipid risk frameworks, that number sits above the threshold most longevity-focused clinicians target. It prompted me to look harder at what was driving it and what it actually meant for someone with my metabolic profile.
The LMHR metabolic pattern changed how I think about what that number means and why monitoring arterial function directly gives me information that the lipid number alone cannot.
ApoB measures particle count. It tells me how much traffic is moving through my arteries. It does not tell me what that traffic is doing to the arterial wall.
For that, I need to look somewhere else.
What my calcium score did and did not tell me
I mentioned earlier that my PCP cleared me six years ago based on a zero calcium score.
What I know now is that the calcium score only measures one thing: calcified plaque. It said nothing about non-calcified plaque, nothing about arterial stiffness, nothing about how my arteries were functioning under the load of decades of high-volume training.
My recent Cleerly scan reaffirmed zero plaque across the board. That is genuinely reassuring data. But reassuring is not the same as complete.
Zero plaque today tells me where I am. It does not tell me what direction I am heading.
Arterial function as the dynamic signal
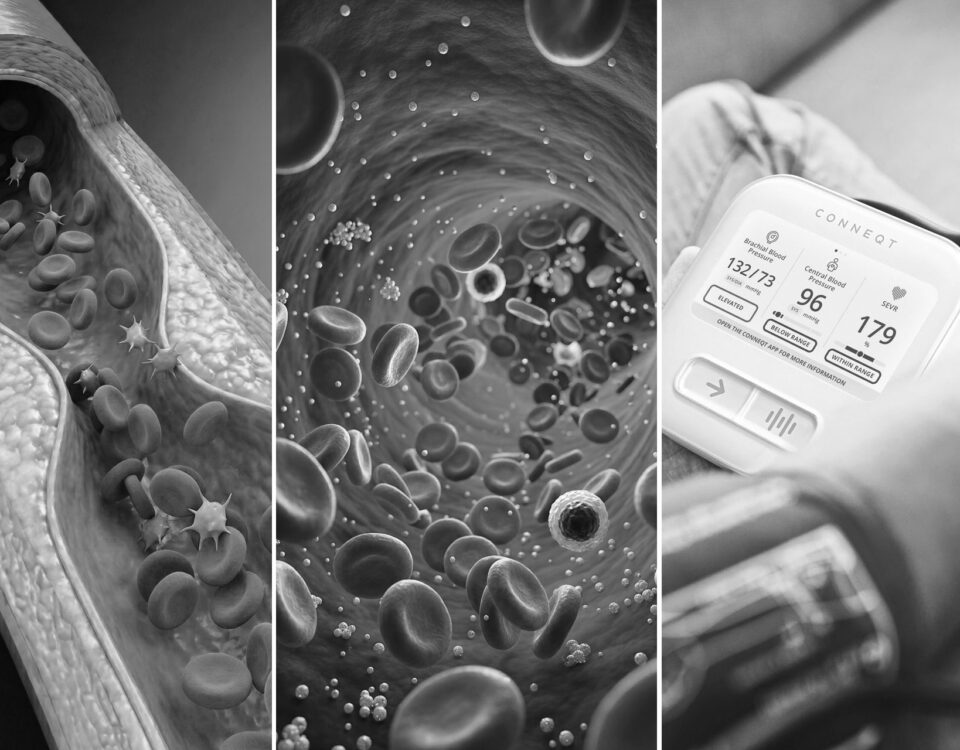
This is where the CONNEQT Pulse fits into my monitoring stack.
Not as a replacement for imaging or lipid markers. As a different kind of signal entirely.
Central blood pressure and arterial stiffness tell me how my arteries are functioning right now, under the ongoing load of elevated particle traffic and high training volume. They are dynamic signals. They change. And tracking them consistently over time tells me something that a single scan or a single blood draw cannot: which direction things are heading.
My arterial function is currently strong. That matters. But I do not treat it as a reason to stop watching.
The question I keep coming back to is this: is my arterial function resilient enough to handle ongoing particle exposure over the next two decades of training?
That is not a question a calcium score answers.
That is not a question a lipid panel answers.
It is the question I am building my monitoring stack around.
What this means for fit athletes thinking about their own risk
If you train consistently at high volume or intensity, the standard risk framework may not be giving you the full picture.
That is not a reason to stop training. It is not a reason to panic about your calcium score or your lipid markers. It is a reason to ask better questions than the ones standard screening is designed to answer.
The questions I now ask look different from the ones I was asking six years ago.
Not just: is my blood pressure normal?
But: what is my ApoB and what is my arterial stiffness trajectory?
Not just: is my calcium score zero?
But: what is driving my lipid markers and what direction are things heading?
The goal is not a clean number on a single test. It is a monitoring stack that actually matches the profile of someone who has trained hard for decades and intends to keep doing so.
The more I have learned about the athlete phenotype and the LMHR pattern, the more I have come to see my cardiovascular monitoring as a conversation between my training and my biomarkers.
Not a single number that tells me everything is fine.
A set of signals that tells me which direction I am heading.
That is a different standard. It is a better one.
If any of this raises specific concerns about your profile, bring it to a clinician familiar with the athlete phenotype. The questions in this article are a starting point, not a substitute for that conversation.
What to read next
If this raised questions about what your arteries are actually doing and how to track the signals that matter, these articles go deeper:
- Three Ways to Look at Your Arteries, And Why You Need All of Them – How structure, flow, and function give you a more complete picture of cardiovascular health than any single test.
- My Cardiovascular Risk Is High, Even Though I’m Fit. Here’s What I’m Doing About It. – The ApoB article that started this conversation. What my numbers showed, what I changed, and why I changed it.
- The Truth About Exercise and Calcium Scores: What the Latest Research Says – A deeper look at what the calcium score actually measures and what the research shows about exercise and CAC.
- Early Signs of Arterial Stiffness: What Changes Before Symptoms Appear – What changes in the arterial wall before symptoms appear, and what consistent measurement can reveal.
Want to explore more? Browse the full library.